Center of Innovation on Disability & Rehab Research (CINDRR)
SPHM Report: Providing Safe VA Care
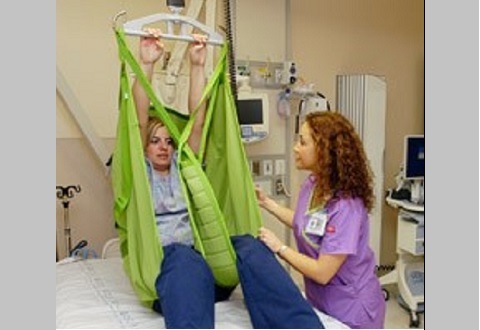
Using a ceiling lift
Safe Patient Handling and Mobility (SPHM) Technologies in Rehabilitation to Improve Patient Mobility and Function
Two CINDRR investigators, Dr. Gail Powell-Cope and Dr. Deborah Rugs, contributed to the most recent VHA Safe Patient Handling and Mobility Survey Report (2016). Dr. Powell-Cope was a member of the 2016 VHA SPHM Survey Technical Advisory Group (TAG). The Survey Report was published in October 2017 and is available at http://vaww.va.gov/haig/haig_pubs3_SPHM.asp.
Safe patient handling and mobility involves the use of assistive devices to ensure that patients can be mobilized safely and that care providers avoid performing high-risk manual patient handling tasks. By using a device made specifically for that activity, care providers can reduce their rate of injury and improve the safety and quality of patient care. The SPHM program at VA utilizes proven methods and the latest specialized devices and equipment to keep Veterans and staff safe when patients need to be moved and lifted.
An important assistive device is a ceiling lift that helps care providers transfer Veterans from beds to stretchers or wheelchairs or can assist them with walking. These portable devices can be moved from room to room. The lifting equipment uses slings or vests to hold patients securely and reduce the risk of slipping, falling or being dropped when walking. This program has led to an over 40 percent reduction in injuries to care providers since 2006. Facility coordinators at each site oversee the program by making sure the right technology and staff is available and that are kept informed of changes and updates.
The purpose of the survey was to help the national SPHM Program monitor the quality of facility SPHM programs by identifying training, resource, and policy needs; assessing compliance with national program guidance; and, identifying factors that are associated with program outcomes. The data gathered in the survey will help to ensure appropriate direction for the SPHM Program and to track changes in national, VISN, and facility status. A total of 140 facilities (100%) responded to the survey. The web-based self-administered survey was available from May 10 - 27, 2016, and was sent through Veterans Integrated Service Network (VISN) offices to facility Directors/Chiefs of Staff to identify targeted respondents for the survey: Facility Coordinator (FC) for SPHM, VISN Point of Contact (POC) for SPHM, Associate Director for Patient Care Services (ADPCS), Facility Safety Manager, and Employee Representative for each Union represented (only this portion was voluntary).
This VHA national survey, completed in collaboration with the Center for Healthcare, Organization and Implementation Research (CHOIR); the National Center for Patient Safety (NCPS); the Occupational Safety, Health and Green Environmental Management System (GEMS) Programs; and the Healthcare Analysis and Information Group (HAIG), examined current practices related to SPHM in the field and identified strengths and barriers to adoption of policies and practices aimed at eliminating manual patient lifting and handling by clinical staff. The results of this survey will be used to advocate a goal of minimal or no lift polices in patient care areas.
Key Findings, SPHM Survey
Among other results, at approximately 57 of 140 facilities, between 91-100% of the front line staff were trained on an ongoing basis on how to use the SPHM equipment and in SPHM concepts. In 69% (97/140) of the facilities, training was accomplished at new employee orientation. Regarding patient lift equipment, 67% (87) sites had 91-100% of their inpatient beds covered with lifts. However, 4% (5) facilities reported that repositioning patients was always conducted using ceiling lifts; a possible explanation for facilities with established SPHM programs reporting substantial numbers of injuries caused by repositioning patients. Some of the reasons for not using ceiling lifts for repositioning were: 1) staff perception of lack of time, 2) lack of co-worker support, 3) lack of unit supervisor expectations, 4) insufficient staff training/knowledge, 5) ceiling lift track configuration not conducive to repositioning tasks, 6) wound care needs, and, 7) lift can’t be used for boosting a patient in bed.
Key Recommendations
- Identify, evaluate, and provide support/site visit to the 10 VA Medical Centers who have not had a program or a SPHM Facility Coordinator in place for over one year
- Integrate SPHM care into existing clinical documentation to be able to report practice changes and access to safe care
- Gain a better understanding of the dynamics contributing to the high turnover rate of Unit Peer Leaders (UPLs) and institute practices that will sustain the designation and retention of UPLs
- Improve Facility Coordinator access to, accuracy of, and reporting of patient handling injury data to monitor and investigate staff injuries locally and nationally
- Include SPHM in the Annual Workplace Evaluation (AWE)



















